
Healthcare System Development for DRG Claims Management
DRG Claims Management, a platform for healthcare-focused insurance providers, helps detect coding errors and reduce reimbursement losses caused by treatment inconsistencies. IT Craft partnered with the company to build a secure claims validation system that streamlines audits and improves accuracy in insurer–provider negotiations.
- Team 5 team members
- Type Platform development
- Industry HealthTech, Insurance
- Platforms Web
About the project with DRG Claims Management
IT Craft developed a unique online healthcare system. This system assists health insurance providers in reviewing treatment claims for errors, abuse, or coding errors. It provides secure means of uploading documents, automated checking, and reporting.
The solution assists insurance firms in obtaining claims located far away, verifying medical codes, locating errors, and producing audit reports with information to discuss with providers.
The client was looking for a cost-effective tool to verify claims. The tool needed to work with sensitive medical information, contain custom algorithms to analyze claims, and support numerous insurance firms.
The objective was to make a system that adheres to HIPAA guidelines, reduces payment risk, simplifies checking for compliance, and accelerates the negotiation process with structured and approved claim information.
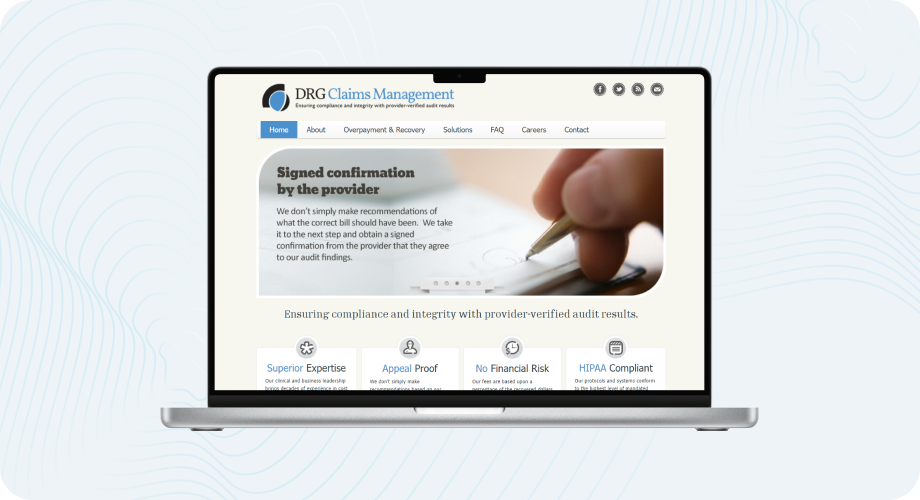
Client’s expectations
- Build a web-based platform to automate the detection of diagnosis and treatment coding errors
- Ensure HIPAA-compliant data handling and document security
- Develop a custom audit algorithm tailored to insurer workflows
- Support remote claims import and streamline cost negotiation with healthcare providers
Technologies:
 ASP.NET MVC
ASP.NET MVC .NET Framework 3.0
.NET Framework 3.0 C#
C# Linq to SQL
Linq to SQL SSIS
SSIS MS SQL 2012
MS SQL 2012 IIS 7
IIS 7 jQuery
jQuery
The client came with deep domain expertise and a clear vision for an automated claims validation system. Our role was to design and implement a secure, scalable solution with custom logic for medical code analysis, optimized workflows, and seamless claim import from distributed sources.
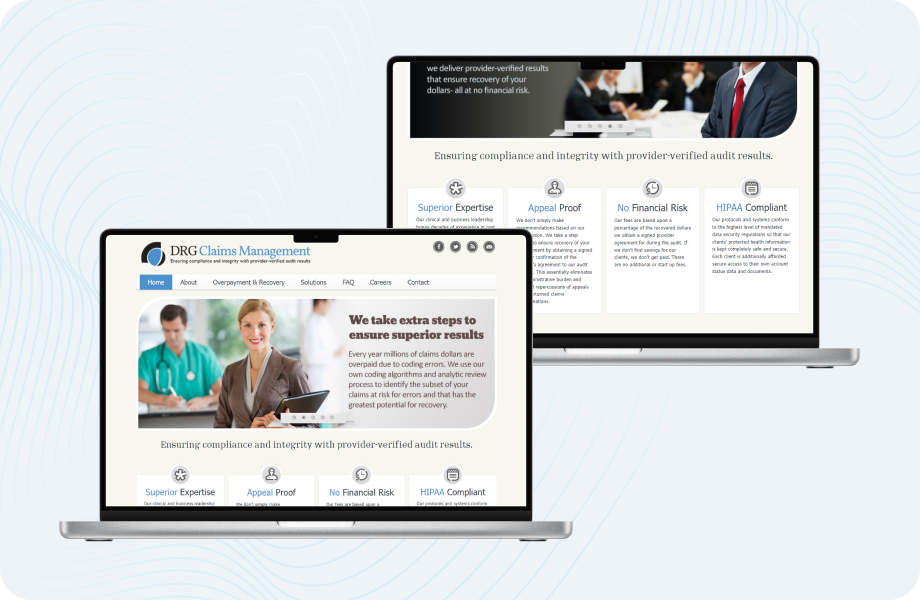
We delivered:
- Cloud-based web application with document upload and role-based access
- Custom-built algorithm for auditing diagnosis and procedure codes
- Secure infrastructure aligned with HIPAA compliance requirements
- UX-focused design for simplified claim management and reporting
- SSIS integration for remote claims data import
- Support for claims status tracking, proof of appeal, and document verification
Results of the collaboration
The DRG Claims Management platform gave insurance providers the tools to reduce compliance risks, recover more reimbursements, and optimize audit processes.
Key outcomes included:
- Accurate claim validation based on automated audit algorithms
- Full compliance with healthcare data privacy and security standards
- Streamlined appeal and reimbursement negotiation workflows
- Increased efficiency for providers and insurers through centralized processing
- Positive client feedback and growing adoption across the target market
To support smarter healthcare operations and reduce reimbursement losses, we delivered a custom claims audit platform tailored to the client’s needs. Explore our healthcare development services expertise to see how we can help transform your healthcare processes.